The company, based in the BioInstrument Center on the Beutenberg campus in Jena, develops and markets three-dimensional, human organ models (so-called organ-on-chip technology or microphysiological systems) to support preclinical research and development as well as to test pharmaceutical substances, chemicals, and food additives. The founders are the biologist Dr. Nancy Blaurock-Möller as well as the biochemists, private lecturer Dr. Alexander S. Mosig, Martin Raasch and Dr. Knut Rennert. They are highly experienced in the development of human, microfluidically-supported in-vitro organ models on biochips.

Team of Dynamic42. Photo. Dynamic42.
Before founding the company, Martin Raasch and Dr. Knut Rennert had already developed human models of the blood vessels, liver, intestine and alveoli in the 'INSPIRE' working group headed by Dr. A. S. Mosig at the University Hospital of Jena (UKJ). "From the very beginning, we considered using these models as marketable alternatives to animal testing in the preclinical phase of drug development," said Knut Rennert describing his motivation. After the foundation of Dynamic42 GmbH, it could be steadily pushed forward. The company is managed by Knut Rennert and Martin Raasch. The team of Dynamic42 develops and commercializes three-dimensional organ models in microfluidic-supported biochips (Organ-on-a-Chip). Dynamic42 also develops in vitro disease and infection models for basic and applied research. These models can be used to conduct mechanistic studies or to test pharmaceutically active substances, e.g. for personalized medicine. In addition to its organ-on-a-chip developments, the company preferentially offers testing services (1).
The scientists and founders have received much recognition for their developments in recent years. In 2018, for instance, they took third place in the "Business Plan" category of the Thuringian Start-up Prize (2) and have just completed a seven-figure start-up financing round (3).
No model without immune cells
The models of Dynamic42 GmbH differ from those of other developers and competing companies in that the immune cells, which are important for the detection of drug side effects, can be integrated into these models both on the tissue side and via the simulated blood flow. They have received several awards for their platform and concept (EY Public Value Award (4), Thuringian Founding Award (5) as well as, under the founding project name "OrganiX", winners of the nationwide business plan competition Science4Life Venture Cup 2017 (6), and the 6th Thuringian Strategy Competition for Innovative Foundings 2017 (7). The modular character of the chip models also allows the combination of two different organ models, e.g. lung and liver for in-depth studies on the toxicity of inhalable therapies. Based on these organ models, it can be determined whether or not a new drug candidate could have side effects in humans before animal experiments are conducted. Thus, on the one hand, drug safety can be increased by using these organ models already in the preclinical phase, and on the other hand, costs and time in drug development can be reduced by reducing the number of clinical trials that have to be terminated in human clinical phases. It is highly likely that the number of animal experiments in drug development will be reduced by these models.
Organ-on-chip models are the test systems of the future
Great hopes are being placed on human organ simulations, cultivated on microfluidic chip systems (see Fig. 1). In the future, it is hoped that they will be able to reduce and, in the long term, replace animal experiments in chemical testing, drug development, and other research issues. In this process, adult cells, e.g. connective tissue cells of the skin, are often reprogrammed (a) into stem cells with the help of specific factors, then further developed into the desired cell type and cultivated. The cells thus obtained carry the genetic information of the donor, which is a great advantage in the research of diseases and the personalized therapies to be developed from them. From the cell arrangements, organ-like tissues are formed, which are introduced into the small cavities of the microfluidic (b) chip for cultivation and examination. A blood-like fluid (nutrient medium with additives to maintain cellular function) is then flushed around the tissue.
Fig. 1: Left: Design of the Dynamic42 chip platform. Right: Fluorescence microscope image of the liver model of Dynamic42; blue: cell nucleus, green: liver cell marker, orange: bile duct marker.
Photos: Dynamic42.
Started about 20 years ago, there are meanwhile a large number of established mini-organ models developed worldwide. They are cultivated on single chips or in a combination of two, four, or far more organ chips. The Wyss Institute in Boston, for example, has recently described a 10-organ approach. In their study, the scientists serially linked the vascular channels of eight different organ chips, including intestine, liver, kidney, heart, lung, skin, blood-brain barrier and brain, using an optimized blood substitute with which all miniaturized organs were supplied. The blood channels of the individual chips were seeded with organ-specific cells. The organ-like tissues and its functions were viable for more than three weeks, making it possible to quantitatively predict the effect of a test chemical (8). Other researchers have also reported a 10-organ chip (9). These studies outline the long-term vision of a "human-on-a chip", however, currently representing highly experimental work. Comprehensive development work is still needed here before the basic functions of a human organism of interest for drug testing can be mapped almost completely without errors in organ interaction.
The small, often spherical, or multi-layered cell arrangements each simulate human organ-like tissue in miniature format. The most important cell types, similar to the in vivo situation, are mainly present. The functionality of such miniature systems (as a single-organ model) has already been shown in countless proof-of-concept and validation studies - but there is still work to be done regarding some details. These include the integration of the immune and hormone systems.
In a time when mankind is threatened worldwide by the coronavirus (SARS-CoV-2) and all the background information is urgently needed for vaccine development, such immunocompetent organ-on-a-chip systems can be of great importance. The coronavirus tightly binds to the receptor called ACE2 (receptor angiotensin-converting enzyme II) of the human lung, heart, kidney, endothelial cells (cell type coating the blood vessels) as well as in the gastrointestinal tract (10, 11, 12, 13, 14). ACE2 acts as a transmembrane protein on the cells. Human in vitro organ models can serve as a complementary testing tool for in-depth investigations in the field of infection biology as well as in the preclinical testing of new therapeutics.
Dynamic42 is a partner of the research campus InfectoGnostics in Jena. Here, procedures for rapid on-site infection diagnostics are developed as well as research into infections such as pneumonia or tuberculosis (15). In cooperation with other partners of the InfectoGnostics research cluster - the Center for Sepsis Control and Care (CSCC), the Leibniz Institute for Natural Product Research and Infection Biology Hans Knöll Institute (HKI), the University Hospital Jena (UKJ) as well as the University of Jena - Dynamic42 GmbH has developed an artificial human model of a pulmonary alveolus ("Alveolus-on-a-Chip"). The artificial pulmonary alveolus provides results for infection research that is closer to the human situation than animal experiments. This may also become a valuable research tool in the current COVID 19 crisis to better understand how the virus works and to evaluate future treatment methods.
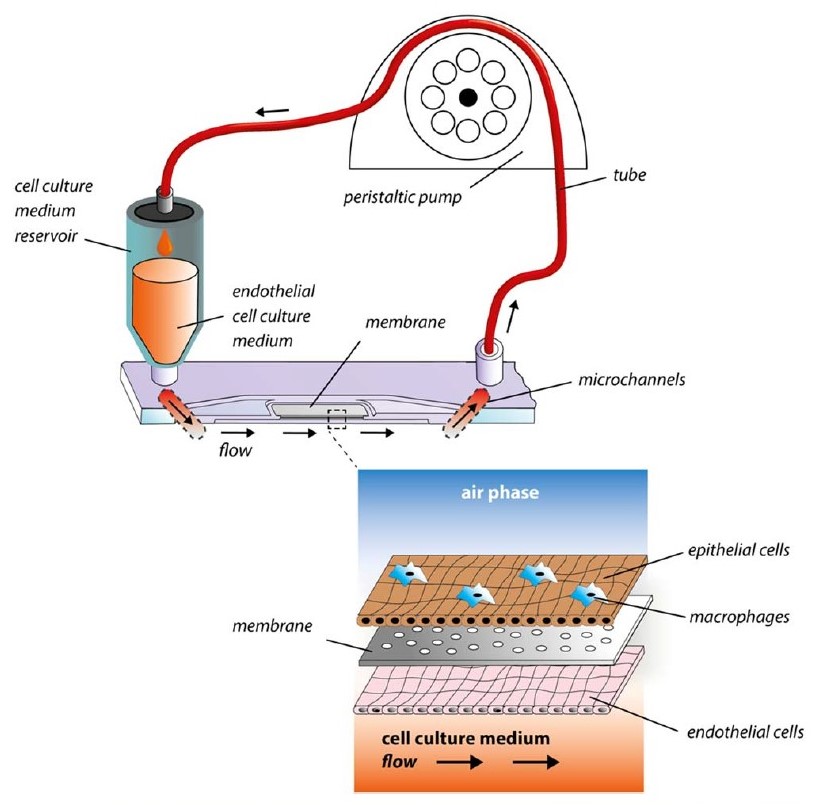
Fig. 2: Microfluidically supported chip model of Dynamic42. An alveolus-on-a-chip is supplied with a blood-like fluid via a pump. The microfluidic chip consists of an upper (air) and a lower (liquid) chamber separated by a porous membrane (Fig. below). The epithelial cells of the alveolus (human NCI-H441 cells) are placed in the upper chamber. After one week of culture, they are co-cultivated with (immune) macrophages. In the lower chamber, endothelial cells (HUVECS) are cultivated in a medium. The compartments are supplied with a fluid from a fluid chamber via microchannels using a peristaltic pump (Fig. above).
Source: Deinhardt-Emmer, S., Rennert, K., Schicke, E. et al. (2020). Biofabrication 12/025012 (16). Creative Commons Attribution 4.0, https://creativecommons.org/licenses/by/4.0/.
Using the alveolus-on-a-chip, the researchers have already been able to show, that the protective inner layer of blood vessels, the endothelium, is damaged, when viruses and bacteria infect the tissue simultaneously (influenza with bacterial superinfection by staphylococci) (16). As a result, pathogens and their toxic metabolites can spread faster in the lungs and lead to sometimes severe pneumonia (15, 16).
The lung: supply and removal organ
The body gains energy by oxidative decomposition of nutrients and thus needs a constant supply of oxygen (17). The lungs are responsible for that. They also ensure the removal of metabolic end products, especially carbon dioxide, and the removal of exogenous particles out of the lungs. They also form an important barrier to the environment.
The so-called respiratory epithelium lines most of the respiratory tract. It consists of several rows of epithelial cells. The inner side (luminal side) of the surface has ciliated cells. Between the normal epithelial cells, there are also glandular cells (so-called goblet cells). They produce mucus, which is released into the lumen at the epithelial surface. The mucus lining is a protective layer that acts as a barrier against bacteria and particles (18). With its help, the passage of particles should be prevented. In healthy people, cilia transport the particles again out of the body. Endocrine cells secrete serotonin and peptides, with which the speed of mucus secretion and cilia beat can be influenced (19). So-called club cells secrete proteins that help to reduce excessive inflammatory processes. Immune cells are also present in the lungs: Alveolar macrophages - migratory phagocytes - take up exogenous substances that have penetrated the alveolar region and render them harmless (20, 21). The "filled" alveolar macrophages are then transported out of the lungs with the mucus (19). The surface of the lung is also colonized by a microbial flora, the so-called microbiota, which can be altered by environmental influences and influences the immune defense (22, 23). When inhaled, the air is initially only passed through a constantly branching system of tubes, at whose end the alveolar ducts are located, which represent the real respiratory area. In the pulmonary alveoli, the gas exchange takes place by diffusion (21).
In the area of the alveoli, the lung is still depicted in many textbooks as a vine. In reality, however, it is supposed to be a sponge-like tissue where the gas exchange between inhaled air and the blood circulation takes place through very fine and specialized tissue walls.
The mechanical interactions between the different types of tissue, the inhaled air, and the liquid film on the tissue are complex (24). The alveoli are composed of single-layered alveolar epithelial cells of type 1 and 2. Type 1 cells form a thin layer of cells in the alveoli, which are located adjacent to the wall cells of the pulmonary capillary cells. They form the blood-air barrier. Here, the exchange of oxygen and carbon dioxide takes place. The alveolar cell type 2 secrete pulmonary surfactant. The surfactant consists of lipids and proteins which reduce the surface tension and prevent the alveoli from collapsing and sticking together on exhalation (25).
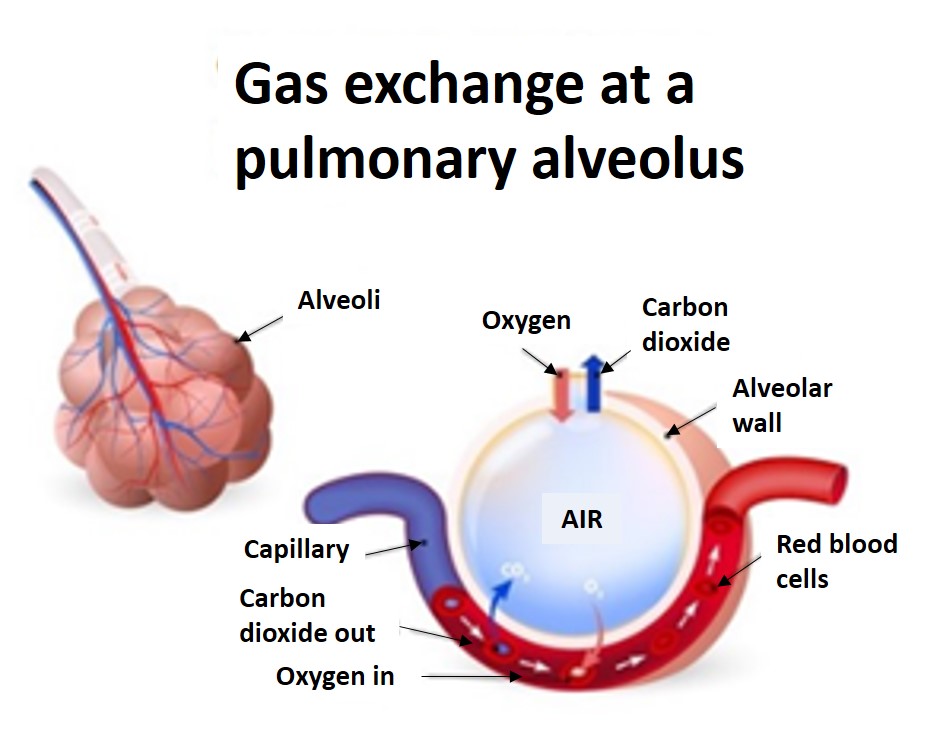
Fig. 3 left: Alveoli with a capillary network. Right: longitudinal section through an alveolus. Gas exchange at the alveoli.
Source: iStock/ttsz
"...The focus for the further development of human organ models should always be on human physiology..."
Photo: Dynamic42.
Martin Raasch and Dr. Knut Rennert are biochemists, who have started their scientific career in basic research. They soon found out that many questions are only addressed in animal models or 2D standard cell cultures. There were no alternatives to animal experiments that were closely related to human physiology and that could have provided added value over the aforementioned models. Therefore, together with private lecturer Dr. A.S. Mosig, the two began almost 10 years ago to develop human models that closely mimic the human physiology. InVitro+Jobs spoke with the two founders of Dynamic42.
InVitro+Jobs: What kind of research does Dynamic42 conduct and which products do you develop?
Dynamic42: First of all, a very warm thank you for the invitation to the interview! Dynamic42 is specialized in the marketing and further development of the so-called "Organ-on-Chip" technology (miniaturized human organ models on biochips). We have already developed models of the human liver, alveolus, and intestine within the research group "INSPIRE" at the University Hospital of Jena before we decided to spin off. And we are further in the process of developing other important organs on the chip, such as a neurovascular unit (c). One of our main interests is the integration of the human immune system into these models. This way it is possible to depict the side effects of active substances much better since the immune system reacts immediately to exogenous substances. We have already integrated monocytes, macrophages as well as T cells into our models, and we are also able to perfuse the immune cells through the models. Similar to the situation in the body, the immune cells can be transported by the blood flow to the target tissue. Soon, we will investigate the effects of neutrophil granulocytes in our organ models. This is generally planned as a long-term project since, in addition to the biological integration of those cells, the analyses in such 3D models are more complex. A publication may not be in sight for at least two to three years. Therefore, a publication of the results cannot be expected in the short term. All in all, we are on a good road in the field of immunocompetence and have already made considerable progress.
InVitro+Jobs: What kind of problems arise during the integration of immune cells?
Dynamic42: Problems arise both during the isolation of the immune cells and their integration into the miniaturized organs. Care must be taken to ensure that they are not activated in advance and release cytokines (c), which would lead to the damage of the surrounding tissue by the immune reaction. For example, one has to make sure that, within a multilayer organ model, the cells only migrate to where they are supposed to be.
InVitro+Jobs: Immune cells seem to be very important for the validity of the models. What is the objective of the EU consortium imSAVAR in this context?
Dynamic42: The scientists involved want to make the already existing organ-on-chip models immunocompetent because the human immune system has so far hardly been considered in many studies on human organ chips. In addition, new 3D models will also be developed. The aim is to evaluate new biomarkers and to be able to study the mode of action of new active pharmaceutical ingredients and treatment methods. One example is the use of genetically modified T-cells in the context of Car-T cell therapy for the treatment of cancer (e). Moreover, this EU project also focuses on adverse (i.e. damaging) mechanisms of action (adverse outcome pathways (f)).
InVitro+Jobs: Can you give us an example of observed side effects that have not been detected with a conventional organ-on-a-chip model?
Dynamic42: For example, in our models, we investigate active pharmaceutical ingredients that were safe in animal experiments, but whose further development had to be stopped in the clinical phase in humans due to side effects. In addition, we compare the effects of this compound with those of an approved drug of a similar type that has received marketing approval. We observe a difference here, for example, in the release of cytokines by tissue-resident (g) immune cells.
InVitro+Jobs: Regarding the models that have currently been validated with the industry: are they incomplete?
Dynamic42: The models will always be incomplete because we will not be able to reproduce a human body in its entirety on the chip, but we will be able to reproduce key functions in a targeted manner. The newly developed models will be more relevant in terms of transferability to humans, compared to 2D cell culture approaches and animal experiments that are currently considered as standards. In principle, the methods and the models, that have been developed so far, will be further refined and adapted. In recent years it has been shown, that 3D models are more predictive than 2D models and organ-on-a-chip models are more predictive than 3D models of single cells, etc. Of course, the developed models also have disadvantages, but they are more helpful than 2D cell cultures under static conditions. The focus for the further development of human organ models should always be on human physiology, that is our motivation. Especially the blood and the immune cells contained in it should therefore not be forgotten in the miniaturized organ systems on the chip.
InVitro+Jobs: That sounds very complicated. Is that why you offer your development as a service to be able to guarantee the quality standards at the end?
Dynamic42: The best way to control the quality of the products is through service. In the long-term, we intend to expand this. However, first, we will provide an in-house platform for standardization. Later, we also want to offer solutions for end-users such as products (organ-on-chip kits) together with training or, in the end, models that are completely ready for shipment. But that is still a dream of the future.
InVitro+Jobs: In cooperation with other InfectoGnostics partners, you have developed an artificial model of a pulmonary alveolus ("Alveolus-on-a-Chip"), based on human cells. Can you briefly describe this?
Dynamic42: We have developed an artificial alveolus by combining a human lung epithelial cell line (NCI-H441) with primary macrophages and endothelial cells. We use a biochip with two cell culture chambers separated by a porous membrane. It simulates the air and blood side of a pulmonary alveolus. Both sides are supplied with nutrient media via tiny microchannels. The alveolar cells are placed on the airside of the chip and are co-cultivated with tissue-associated, pre-differentiated macrophages. On the blood side, we cultivate blood vessel endothelial cells on the chip. As "blood" we use nutrient medium, that is adapted to endothelial cells and immune cells of the blood (monocytes). At the moment, real blood would otherwise form clumps in the tiny channels. However, it is also mixed with donor serum, so that important human serum proteins are also included. In the published study (16), viruses and bacteria (staphylococci) - simulated influenza with bacterial superinfection - were added via the airside and examined to see, whether the tissue created in the alveolar model was affected. It was shown that the protective inner layer of the blood vessels, the endothelium, is damaged. Among other things, the focus was on whether and how an immune reaction of the alveolar macrophages proceeds after pre-incubation of influenza and subsequent addition of staphylococci.
If they are not immediately caught on the surface by the macrophages, exogenous particles such as viruses or bacteria can penetrate into deep lung areas through the airstream. For the case of particle removal, an exogenous particle would be enclosed in an air bubble by the surfactant layer. These particles entrapped by surfactant molecules are then recognized by the macrophages, which leads to particle absorption and their subsequent destruction (26).
InVitro+Jobs: Is it possible to use your model for Covid-19 research?
Dynamic42: In principle, it is possible to investigate the infection behavior of the SARS-CoV-2 pathogen. In the future, we also want to use this model for drug testing. We already have interested customers from the pharma industry and we have already submitted applications for further development of the lung model. However, it would be necessary to work in a biological safety level 3 laboratory.
InVitro+Jobs: How many immune cell types can you integrate into your Alveolus-on-a-Chip models?
Dynamic42: Depending on the research question, single or mixed populations of immune cells can be included in addition to the alveolar macrophages already described, such as neutrophil granulocytes and certain T-cells.
InVitro+Jobs: What is the difficulty in integrating T cells?
Dynamic42: T-cells have to be permanently perfused (i.e. flowed around with fluid) and you need to have a high number of these cells in stock to be able to detect effects. It also takes a long time for T-cells to adhere to the tissue or for their effects to become visible. In addition, in the end, one has to be sure that the observed effect is also linked to the T-cells and not to an artifact.
InVitro+Jobs: Are there any plans to combine the different organ chips you have developed with liver, intestinal, and alveolar cells into a multiorgan-on-a-chip?
Dynamic42: Yes, in principle it is. But only two or three organs with each other. For example, we are currently working on a gut-liver-axis model, whose organs are connected via the bloodstream. The model is currently being standardized. However, for the time being, it should not be more than three organ types, because otherwise there will be too many random variants, that can accumulate depending on the number of connected organ types. For this purpose, mathematical models must be developed, that can calculate and extract the influence of these unknown factors. However, we currently do not have such a mathematical model.
InVitro+Jobs: To what extent can animal experiments be replaced with your models?
Dynamic42: This depends on the field of application of the model. It is not possible to show this in general percentages. In the long-term, we hope to be able to replace 10% of the preclinical animal experiments in drug development with our models and possibly, even more, depending on the progress of technology development. We are aiming for our human models to be recognized and widely used as an alternative to animal testing. In drug development, organ-on-a-chip technology can already be used to obtain preliminary information, which at least reduces the number of animal experiments.
InVitro+Jobs: Thank you for the interview.
Literature:
(1) https://dynamic42.com/
(2) https://www.cluster-thueringen.de/aktuelles/news/news-details/news/thueringer-gruenderpreis-2018-in-hoehe-von-75-000-euro-vergeben/
(3) https://www.bm-t.de/2020/das-jenaer-biotechnologieunternehmen-dynamic42-wirbt-sieben-stelliges-investment-ein/
(4) https://eypva.com/de/award/award18/dynamic42/
(5) https://www.thex.de/blog/thueringer-gruenderpreis-2018-das-sind-die-gewinner/
(6) https://www.science4life.de/preistraegerarchiv/?preis_year=2017
(7) https://www.thex.de/innovativ/2017/10/18/innovative-unternehmensstrategien-aus-thueringen-praemiert/
(8) Novak, R., Ingram, M., Marquez, S. et al. (2020). Robotic fluidic coupling and interrogation of multiple vascularized organ chips. Nat Biomed Eng 4, 407–420. https://doi.org/10.1038/s41551-019-0497-x
(9) https://cn-bio.com/cn-bio-to-bring-10-organs-together-on-a-chip-2/
(10) Markus Hoffmann, Hannah Kleine-Weber, Simon Schroeder, Nadine Krüger, Tanja Herrler, Sandra Erich-sen, Tobias S. Schiergens, Georg Herrler, Nai-Huei Wu, Andreas Nitsche, Marcel A. Müller, Christian Drosten & Stefan Pöhlmann (2020). SARS-CoV-2 Cell Entry Depends on ACE2 and TMPRSS2 and Is Blocked by a Clini-cally Proven Protease Inhibitor. Cell 181: 1-10. April 16, 2020. https://doi.org/10.1016/j.cell.2020.02.052
(11) Zhou P., Yang X., Wang G. et al. (2020). A pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature 579: 270–273. https://www.nature.com/articles/s41586-020-2012-7?proof=trueMay%2F
(12) C. Tikellis & M. C. Thomas (2012): Angiotensin-Converting Enzyme 2 (ACE2) is a Key Modulator of the Renin Angiotensin System in Health and Disease. International journal of peptides 2012, Article ID 256294. https://www.hindawi.com/journals/ijpep/2012/256294/
(13) R&D Systems (2020). ACE-2: The Receptor for SARS-CoV-2 https://www.rndsystems.com/resources/articles/ace-2-sars-receptor-identified
(14) Varga, Z., Flammer, A. J., Steiger, P., Haberecker, M., Andermatt, R., Zinkernagel, A. S., Mehra, M. R., Schuepbach, R. A., Ruschitzka, F. & Moch, H. (2020). Endothelial cell infection and endotheliitis in COVID-19. The Lancet https://doi.org/10.1016/ S0140-6736(20)30937, https://www.thelancet.com/action/showPdf?pii=S0140-6736%2820%2930937-5
(15) https://www.infectognostics.de/infektionsdiagnostik/aktuelles/details/news/superinfektionen-bei-influenza-jenaer-lungenblaeschen-chip-zeigt-wie-bakterien-und-viren-zellbarrie.html
(16) Deinhardt-Emmer, S., Rennert, K., Schicke, E., Cseresnyés, Z., Windolph, M., Nietzsche, S., Heller, R., Siwczak, F., Haupt, K. F., Carlstedt, S., Schacke, M., Figge, M. T., Ehrhardt, C., Löffler, B. & Mosig, A. S. (2020). Co-infection with Staphylococcus aureus after primary influenza virus infection leads to damage of the endothelium in a human alveolus-on-a-chip model. Biofabrication 12/025012, https://doi.org/10.1088/1758-5090/ab7073
(17) Thews, G. & Vaupel, P. (2005): Vegetative Physiologie. Springer Verlag, Heidelberg.
(18) http://flexikon.doccheck.com/de/Respiratorisches_Flimmerepithel
(19) Alberts, B., Johnson, A., Lewis, J., Raff, M., Roberts; K. & Walter, P. (2011): Molekularbiologie der Zelle. 5. Auflage. Verlag Wiley Blackwell.
(20) Gordon, S., Daneshian, M., Bouwstra, J. et al (2015): Non-Animal Models of Epithelial Barriers (Skin, Intestine and Lung) in Research, Industrial Applications and Regulatory Toxicology. ALTEX 32 (4): 327-378. DOI: http://dx.doi.org/10.14573/altex.1510051.
(21) Wennemuth, G. (2012): Taschenatlas Histologie. Urban & Fischer, München.
(22) Gollwitzer ES, Saglani, S, Trompette A, Yadava K, Sherburn R, McCoy KD, Nicod LP, Lloyd CM & Marsland BJ (2014): Lung microbiota promotes tolerance to allergens in neonates DP-L1. Nat Med. 20 (6) :642-647. doi: 10.1038/nm.3568.
(23) Yun, Y, Srinivas, G, Kuenzel, S, Linnenbrink, M, Alnahas, S, Bruce, KD, Steinhoff, U, Bainesm JF & Schaible UE (2014): Environmentally Determined Differences in the Murine Lung Microbiota and Their Relation to Alveolar Architecture. PLOS ONE December 3, 2014. DOI: 10.1371/journal.pone.0113466
(24) https://science.apa.at/rubrik/medizin_und_biotech/Digitales_Lungenmodell_fuer_schonendere_kuenstliche_Beatmung/SCI_20200423_SCI39371351254274450
(25) Speckmann, E.-J., Hescheler, J. & Köhling, R. (2008): Physiologie. Urban & Fischer Verlag, München.
(26) Schicke, E., Cseresnyés, Z., Rennert, K., Vau, V., Haupt, K. F., Hornung, F., Nietzsche, S., Swiczak, F., Schmidtke, M., Glück, B., Koch, M., Schacke, M., Heller, R., Mosig, A. S., Figge, M. T., Ehrhardt, C., Löffler, B. & Deinhardt-Emmer, S. (2020). Staphylococcus aureus Lung Infection Results in Down-Regulation of Surfactant Protein-A Mainly Caused by Pro-Inflammatory Macrophages. Microorganisms 8/577. doi:10.3390/microorganisms8040577
Glossary:
(a) Cell reprogramming: With the help of transcription factors, it is possible to reprogramme somatic cells into a pluripotency state, the developmental state similar to embryonic stem cells (https://www.biocompare.com/Understanding-the-Key-Epigenetic-Processes-in-Cellular-Reprogramming-and-Pluripotency-Building-Future-Therapeutics-6/)
(b) microfluidic: Behaviour of small quantities of liquid in confined spaces. (https://en.wikipedia.org/wiki/Microfluidics)
(c) neurovascular unit: Blood capillaries in which each of the fine blood vessels consists of endothelial cells connected by extremely dense tight junctions, surrounded by pericytes and astrocytes. Together they form the blood-brain barrier (BBB), also called neurovascular unit (https://academic.oup.com/neurosurgery/article/82/6/770/3988111).
(d) cytokines: Inflammatory mediators
(e) car cell therapy: https://www.novartis.com/our-focus/cell-and-gene-therapy/key-focus-areas/car-t/car-t-patients
(f) Adverse Outcome Pathways: https://de.wikipedia.org/wiki/Adverse_Outcome_Pathway, https://www.oecd.org/chemicalsafety/testing/adverse-outcome-pathways-molecular-screening-and-toxicogenomics.htm
(g) tissue-attributed: attributed to a special tissue







 Dr. rer. nat.
Dr. rer. nat. Menschen für Tierrechte - Tierversuchsgegner Rheinland-Pfalz e.V.
Menschen für Tierrechte - Tierversuchsgegner Rheinland-Pfalz e.V.