Hesperos work group in Orlando, Florida. Back row, center: Chief Scientist Prof. Dr. James Hickman.
Photo: Hesperos Inc.
In Germany, around four million patients are suffering from a rare disease. Only very few of them profit from drug therapy. One reason for this is that the mechanisms of action in rare diseases are often unknown. Such diseases have traditionally been researched with mice, less frequently with zebrafish or rats. However, animals do not develop such diseases at all; only a similar disease phenomenon can be genetically engineered in an animal. Correspondingly, new treatments are rarely found. Therefore, organ and human-on-a-chip developments such as those of the start-up Hesperos Inc. make sense, particularly, because the development of animal models is expensive and the cost of developing a drug is very high due to the small number of patients.
Rare diseases
It is estimated that approximately 30 million patients across Europe suffer from a rare disease. A disease is considered rare if it affects no more than five people per 10,000 population; in the U.S., the total number may not exceed 200,000. 6,000 to 8,000 rare diseases are known, and scientists disagree on the number (1). The bad news is that drug therapy is available for only 100 of the 8,000 diseases (2). One of the reasons is that the disease mechanisms are often unknown. Rare diseases are extremely diverse and complex. It can be certain forms of cancer, diseases of the cardiovascular system, the nerves, metabolism, or autoimmune diseases (3). As they are of predominantly genetic origin, they can occur early in childhood, lead to health impairments, and frequently shorten life expectancy (2). Example: The neuronal ceroid lipofuscinosis (NCL) bundles a group of neurodegenerative diseases with similar clinical symptoms such as dementia, loss of vision as well as epilepsy in childhood and adolescence. Typical signs of the disease appear between the second and fourth years of life (4). In this process, a fatty, brownish substance (ceroid lipofuscin) is deposited in the cells of the CNS, leading to neuronal cell death (5, 6). Such cells of the central nervous system can be developed into a patient-specific model that carries all the hallmarks of the disease to explore drug effects.
Patients with the rare disease neuronal ceroid lipofuscinosis (NCL) are often confined to a wheelchair from late childhood.
Photo credit: iStockphoto.
Because the patients' illnesses are so rare, pharmaceutical companies are not willing to invest in this research under normal market conditions. Incentives are therefore needed if drugs are to be successfully developed (7). Drug developers are encouraged by the European regulation on orphan drugs, which has been in force since 2000. In the United States, the Orphan Drug Act (ODA) has been in place since 1983 and also provides incentives for research into neglected diseases that would otherwise not cover development costs (8). Germany adopted a National Action Plan on Rare Diseases in August 2013 (1). In the European Union (EU), 121 medicines are currently available for the treatment of rare diseases (9).
Controversial animal models for research into rare diseases
The fundamentals of rare diseases, as well as possible drugs, are traditionally investigated with mice, less frequently with zebrafish or rats. Once a substance has been found, legally required animal tests follow, including tests with non-human primates (e.g., Javanese monkeys).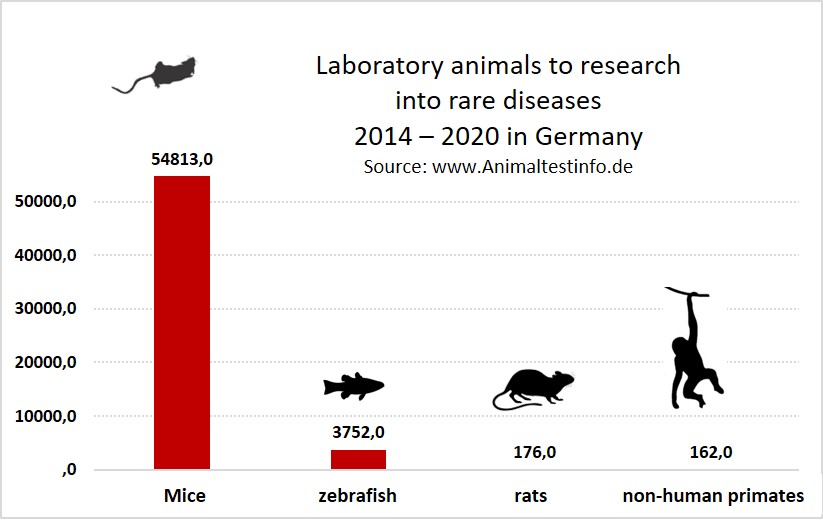
Mainly genetically engineered mice are used for research into rare diseases. Non-human primates (e.g. Javanese monkeys) are used in legally prescribed animal experiments of preclinical drug development.
Source: www.Animaltestinfo.de (10)
However, animal models often fail to replicate the responses to drugs observed in the human body because of species differences. Animals do not develop these diseases at all; only a similar disease phenomenon can be genetically engineered in the animal - with corresponding inaccuracies. Animal experiments are also often associated with severe stress for the animals. Sandhoff disease, for example, is based on a mutation at the HEXB gene, resulting in the absence or deficiency of two subunits of an important enzyme (hexosaminidase). As a result, water-insoluble fats accumulate, especially in nerve cells. The result is a stagnation in the child's development, with learned skills being lost again later. Blindness can also result. Affected children usually die at the age of 4 years (11, 12).
A genetically engineered Sandhoff disease mouse model is being used to investigate brain endothelium-specific gene therapy. However, it is not without controversy in the scientific community: The genetically engineered (hexb-/-) Sandhoff mouse, for example, shows severe motor dysfunction and a short lifespan, which, in contrast to humans, can be explained by an alternative degradation pathway of GM2 ganglioside in the mouse model. Besides, hyperactivity of the immune system is thought to be partly responsible here (13, 14, 15, 16).
An opportunity for non-animal methods
For developers of organ-on-a-chip or human-on-a-chip models, the simulation of rare diseases is an opportunity. This is because it has the potential to discover patient-specific treatment options, which can reduce costs and time as well as increase drug approval rates (17). This has already been achieved in individual cases: The rare Leigh syndrome cardiomyopathy has already been able to be successfully treated after a suitable drug was found on a personalized in vitro disease model (18, 19, 20). Hesperos scientists themselves recently studied amyotrophic lateral sclerosis (ALS) using induced pluripotent stem cell (iPSC)-derived motor neurons to evaluate a holistic treatment in a neuromuscular junction model (21). Amyotrophic lateral sclerosis (ALS) is a progressive neurodegenerative disease that is characterized by selective loss of motor neurons in spinal cord and in cranial nerve nuclei of the brainstem and motor cortex of the brain (24). Muscular atrophy, muscle weakness, spasticity, and paralysis occur, leading to death by progressive atrophy of the respiratory muscles. The cause of the disease, with the exception of rare hereditary forms, is as yet unknown.
In another study, the scientists used an in vitro model with human skeletal muscles on a muscle function chip. The skeletal muscles were developed from induced pluripotent stem cells from ALS patients. The scientists compared the characteristics of the patient skeletal muscles with those of healthy volunteers. The skeletal muscles of the ALS patients had mutations in a gene that codes for an important enzyme (superoxide dismutase 1). In their model, they were able to show that this leads to a reduced fusion capacity of the muscle, a shortening of the myotube length, and the reduced formation of important acetylcholine receptors. ALS muscles also showed, for example, reduced contractile force and impaired muscle fiber metabolism (21).
Hesperos Inc. has targeted rare disease research as one of its primary focus areas. The Orlando-based start-up develops pump-free multi-organ microphysiological systems (human-on-a-chip systems) suitable for rare disease research as they can be custom designed for individual diseases. The company was founded by professors Dr. Michael Shuler and Dr. James J. Hickman, who have many years of experience in body-on-a-chip research, with Dr. Shuler considered the inventor of the field. Hesperos has already constructed microfluidic systems with human cardiac, muscle, glial, endothelial, hepatocyte, bone marrow, cancer, immune and epithelial cells and completed validation studies with industry (22). The design of their microfluidic chip systems is pumpless to eliminate the need for pumps and tubing which simplifies the platforms, eliminates bubble formation, and makes it a low volume system that allows analysis of both parent and its metabolites if a liver model is included.
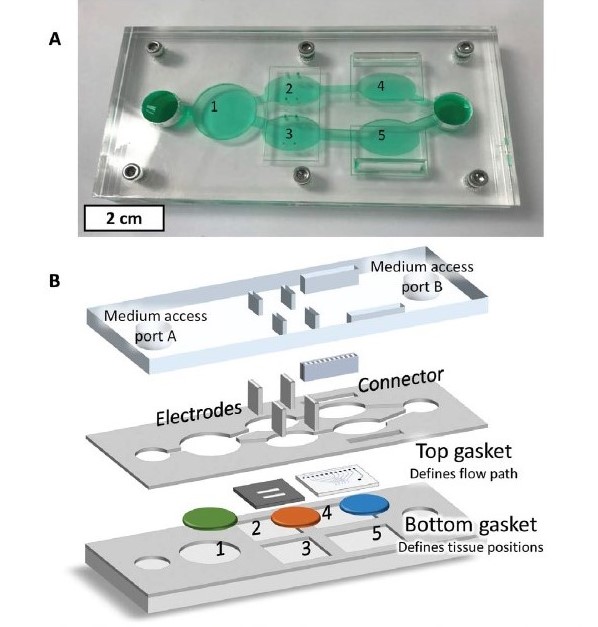
Example of a developed multi-organ system.
A) 5-chamber multiorgan system in an overview.
B) Chamber 1 contains liver cells, chambers 2 and 4 are heart cells on cantilevers and multielectrode arrays (MEAs), respectively, chambers 3 and 5 were used for two different cancer cell lines in this case. Test compounds are added to the medium in port A and pass through the liver first to simulate the first-pass metabolism.
Source: McAleer et al (2019). Science Translational Medicine 11/497, DOI: 10.1126/scitranslmed.aav1386
(with kind permission of AAAS)**
One example of the wealth of developments at the Hesperos start-up is the so-called cantilever chip: it consists of 32 microscopically small silicon cantilevers where heart or muscle cells can be cultured on the cantilever surface. A laser and photodetector system is used to record the cellular contraction at the cantilevers, which are set into flexion by the slightest cell movement. When a test substance affects a muscle cell, the contraction deviation is accurately recorded in magnitude, time and duration. In a combined model, multi-electrode arrays are used to measure the electrical activity of cells, primarily cardiac and neuronal cells, and the cantilever model is used to measure stress contractions of cardiac muscle cells as well as skeletal muscle with the photodiode laser and detector system (23).
"... a simple, effective, and also relatively inexpensive way to research rare diseases..."
Research into rare diseases is unattractive to pharmaceutical companies. Because of the considerable effort involved and the small number of patients affected, the costs and benefits for the companies are simply not in proportion. In addition, there is little funding available for research - and little or no so-called animal models on which to study them. For this reason, the research area of rare diseases is an ideal example to show the advantages that complex animal-free methods, such as human-on-a-chip technology, offer. We spoke with Chief Scientist Prof. Dr. James J. Hickman about the potential of these animal-free techniques for rare disease research and beyond.
InVitro+Jobs: Animal models are still primarily used to research diseases and therapies. What is the situation with rare diseases?
Prof. Hickman: There are over 7,700 known rare diseases, compared to only about 400 active research programs. This is because, due to the small number of patients, in most cases, minimal funding is available for research into rare diseases. Thus, there are only a few animal models in existence for rare diseases and, in many cases, because they are humanized models they are prohibitively expensive. In addition, for most rare diseases, there are no animal models at all due to technical limitations.
InVitro+Jobs: Can you explain in simple words how human-on-a-chip technology works in this field?
Prof. Hickman: It is a simple process to create stem cells from patients with a rare disease, differentiate the cells into the cells most affected or use serum samples from patients to develop phenotypic models that differ from the healthy subject (wild type) in some key function. Any molecules* that can enhance the performance and bring it closer to the wild type would have the potential to treat the disease.
InVitro+Jobs: So, science in this field is practically forced to investigate these diseases using animal-free methods?
Prof. Hickman: Human-on-a-chip technology is a simple, effective and relatively inexpensive way to research rare diseases. This automatically leads to a reduction in animal testing in this field through chip technology.
InVitro+Jobs: If we turn it around, could we say that the existence of animal disease models even hinders research and the effective development of certain therapies? Because, if an animal model exists, the chip technology is not used at all and cannot prove itself as a method.
Prof. Hickman: No, even if an animal model exists, the HoaC technology can help reduce and refine those experiments and can potentially be shown during such experiments to be a better model than the animals. So, if an animal model exists, it does not preclude the application of an HoaC technology to the rare disease.
InVitro+Jobs: Which rare diseases can already be explored with the Human-on-a-Chip (HoaC) technology?
Prof. Hickman: At Hesperos, we have a number of promising drug candidates for different rare diseases researched with HoaC technology and believe that the majority of rare diseases can be addressed using HoaC technology. We have already filed one investigational new drug application for a rare disease using this methodology and have numerous others under development.
InVitro+Jobs: What other advantages do HoaC methods offer for rare disease research?
Prof. Hickman: Most rare disease animal models do not currently exist or are not feasible for technical or financial reasons. In addition, it is probably a better model for drug efficacy research compared to other techniques because we can create phenotypic models using real patient samples. The advent of stem cell technology makes it straightforward to transform patients' cells into stem cells which can then be differentiated into the affected cells. In other rare diseases, just plasma from blood samples will be sufficient, for example, for some immune disorders where the antibodies causing the disease are in the blood.
InVitro+Jobs: What rare diseases can already be investigated with HoaC at Hesperos?
Prof. Hickman: Hesperos is currently focusing mainly on neurological rare diseases for both central nervous system and peripheral nervous system disorders. We are also investigating lysosomal storage diseases as well as liver and heart phenomena.
InVitro+Jobs: Could it be said that more funding for chip technology would also lead to more therapies for affected patients?
Prof. Hickman: Yes, I believe this is the case, especially if the funding is targeted at rare diseases.
InVitro+Jobs: How are developers supported in rare disease research, such as from the Orphan Drug Act (ODA)?
Prof. Hickman: Hesperos at this time has not been able to apply directly to this program. However, it is working with companies that have utilized this route to raise capital or obtain resources that otherwise would not have been available to them for rare disease research.
InVitro+Jobs: What are the difficulties in developing a chip technology for rare diseases?
Prof. Hickman: The primary limitation of rare disease research at this point is funding, as well as access to patient samples. There are also some rare diseases where the usage of HoaC technology is not optimal. But because we can build networked multi-organ systems individually, we have a wide range of disease indications that we can address.
InVitro+Jobs: Have the results of researching a rare disease with HoaC already led to the development of a drug?
Prof. Hickman: I cannot speak for other companies or research efforts in rare diseases, but I am not aware of any efforts yet that have resulted in an approved drug. However, this is not because of the performance of the technology, but because it has only recently been commercialized. Research into rare diseases using chip technologies is growing rapidly. At Hesperos, we have a number of promising candidates for different rare diseases and we have one molecule that we worked on with a pharmaceutical company Bioverativ, that generated excellent results in one of our functional models. That enabled an investigational new drug application to be filed with the FDA based primarily on those results.
InVitro+Jobs: Have developments led to collaborations with the pharmaceutical industry?
Prof. Hickman: Yes, we have established collaborations with small, medium and large size pharmaceutical companies as well as government, academic and not-for-profit organizations.
InVitro+Jobs: Are there already courses at your university UCF where students can learn in vitro modeling of rare diseases?
Prof. Hickman: Unfortunately, the technology is too new to have generated interest from the administration at UCF that would enable the establishment of courses in this area of research.
InVitro+Jobs: What do you think is the potential of chip technology beyond rare disease research?
Prof. Hickman: We are focused on rare diseases because we believe it is an unmet need, however, we and other microphysiological system companies are also working on more mainstream diseases such as heart disease, Alzheimer’s and diabetes.
InVitro+Jobs: Thank you for the interview.
* Molecule: potentially pharmaceutically active substance under investigation.
** Readers may view, browse, and/or download material for temporary copying purposes only, provided these uses are for noncommercial personal purposes. Except as provided by law, this material may not be further reproduced, distributed, transmitted, modified, adapted, performed, displayed, published, or sold in whole or in part, without prior written permission from the publisher.
References:





 Dr. rer. nat.
Dr. rer. nat. Menschen für Tierrechte - Tierversuchsgegner Rheinland-Pfalz e.V.
Menschen für Tierrechte - Tierversuchsgegner Rheinland-Pfalz e.V.