
Point of attack of chemical carcinogens: DNA
Graphic: Darwin Laganzon, Pixabay
Cancer is one of the most serious conditions worldwide: it is the second cause of premature death before the completion of the 65th year of life, comprising almost 20 percent of all cases in Europe3 In Germany alone, over 230,000 people succumbed to cancer in 2018.4 However, around 37 percent of these cases could be preventable or at least controllable; causes include tobacco consumption, obesity, lack of exercise and extensive sunbathing.5 However, tumors can also be of genetic origin or caused by ionizing radiation, viruses or chemical substances (single substances or mixtures). The target is the basic genetic material (genome) of the cell, the deoxyribonucleic acid (DNA). The DNA can also be damaged by an organism own metabolism (by so-called reactive oxygen molecules for example from the respiratory chain) in form of base loss, base modification or DNA single or double-strand breaks.
Researchers suspect that there occur 5,000 so-called DNA strand breaks per hour in the cell alone.6 However, under normal circumstances, the cell is capable of repairing the damage itself, unless its systems are impaired as a result of poisoning, extensive exposure to ultraviolet light or ionizing radiation, or by age. Maybe these systems are indeed even affected by mutation themselves.
To a certain degree, environmental chemicals can play a role as well. This is why the health protection of people involved in the production, trade or use of chemicals, like e.g. pesticides or their residues, must be guaranteed. For approval, these substances have to be tested first for its potential to cause cancer (carcinogenicity).7
Graph of a DNA-Helix with strand break
Graphic: PhonlamaiPhoto, iStockphoto
Genotoxicity, Mutagenicity, Carcinogenicity
Genotoxic: substances that have damaging effects on the genome. They can lead to mutations or increase the error rate during the doubling of the DNA during each cell division. Genotoxicity is therefore not necessarily associated with mutagenicity.8
Mutagenicity must be distinguished from genotoxicity: mutagens are substances or radiation that cause a change in the DNA which leads to a change in the genetic makeup. However, a mutation does not (yet) mean tumor formation.
A carcinogen is a substance that can convert a cell into a tumor cell; it has tumor- generating potential.9 This takes place through a change in the DNA and the initiation of tumor development. Due to their toxic effects, a distinction is made between genotoxic and non-genotoxic carcinogens. Genotoxic carcinogens react directly with the DNA of the cell, finally resulting in a mutation. Non-genotoxic substances work through secondary mechanisms that do not involve any direct interaction with DNA. They do not trigger any short-term mutations in eukaryotic and prokaryotic mutation tests and do not induce any direct DNA damage in the target organ.10 As a consequence, they cannot be detected using genotoxicity tests. Non-genotoxic carcinogens also include substances which lead to epigenetic changes. They react i.e. also with proteins or immune cells, as is the case with asbestos. 6, 10
A tumor means first and foremost a growth or swelling due to increased cell division of tissue. Only malignant tumors are called cancer. Whether the growth is benign, semi-benign (semi-malignant), or malign (malignant) depends on its growth behavior.11 With the exception of blood cancers, such tumors grow invasively into the surrounding tissue and destroy it.12 They can also disseminate into more distant regions of the body and form metastases.
Gradual Development of Tumors after a long Latency Period
Most of the time, carcinogenic effects occur a long time after the relevant exposure. The development of cancer occurs in three stages: tumor initiation, tumor promotion and tumor progression.13
The first step of cell mutation is known as initiation. Individual, dividing viable cells (stem cells) mutate, resulting in an irreversible, inheritable alteration, which are passed on to all cells resulting from the cell division. The DNA damage is passed on from cell generation to cell generation.6
During the promotion stage, the process of tumor development is accelerated. The selection of tumor-initiated cells accelerates. So-called pre-neoplasms develop (benign tumors). Injuries, inflammatory processes or a hormonal stimulus can promote this development.6 The last step, progression, means the transformation from benign to malignant tumors, including genetic and phenotypic changes within the cells. In the end, the inactivation of the genes coding for repair enzymes proves to be fatal. Mutations accumulate in the cells. This results in increasingly aggressive or invasive cells that can divide indefinitely. Metabolism is reprogrammed in favor of tumor nutrition, and blood vessels form in the tumor supplying it with oxygen and nutrients. The cells become resistant to attacks of the immune system, programmed cell death (apoptosis) does not work anymore. Metastases forms migrate into other tissues and there, in turn, develop their destructive work.6
Legal Requirements
Regulatory requirements for testing the carcinogenicity of chemicals vary depending on the properties and production quantities of the chemical. In vitro genotoxicity tests come first. If these tests are positive, the result is checked in vivo and supplemented with tests in mammals.10 Genotoxicity tests are carried out to determine whether the test substance causes mutations (in genes, chromosomes or in the genome).
Genotoxicity tests according to OECD
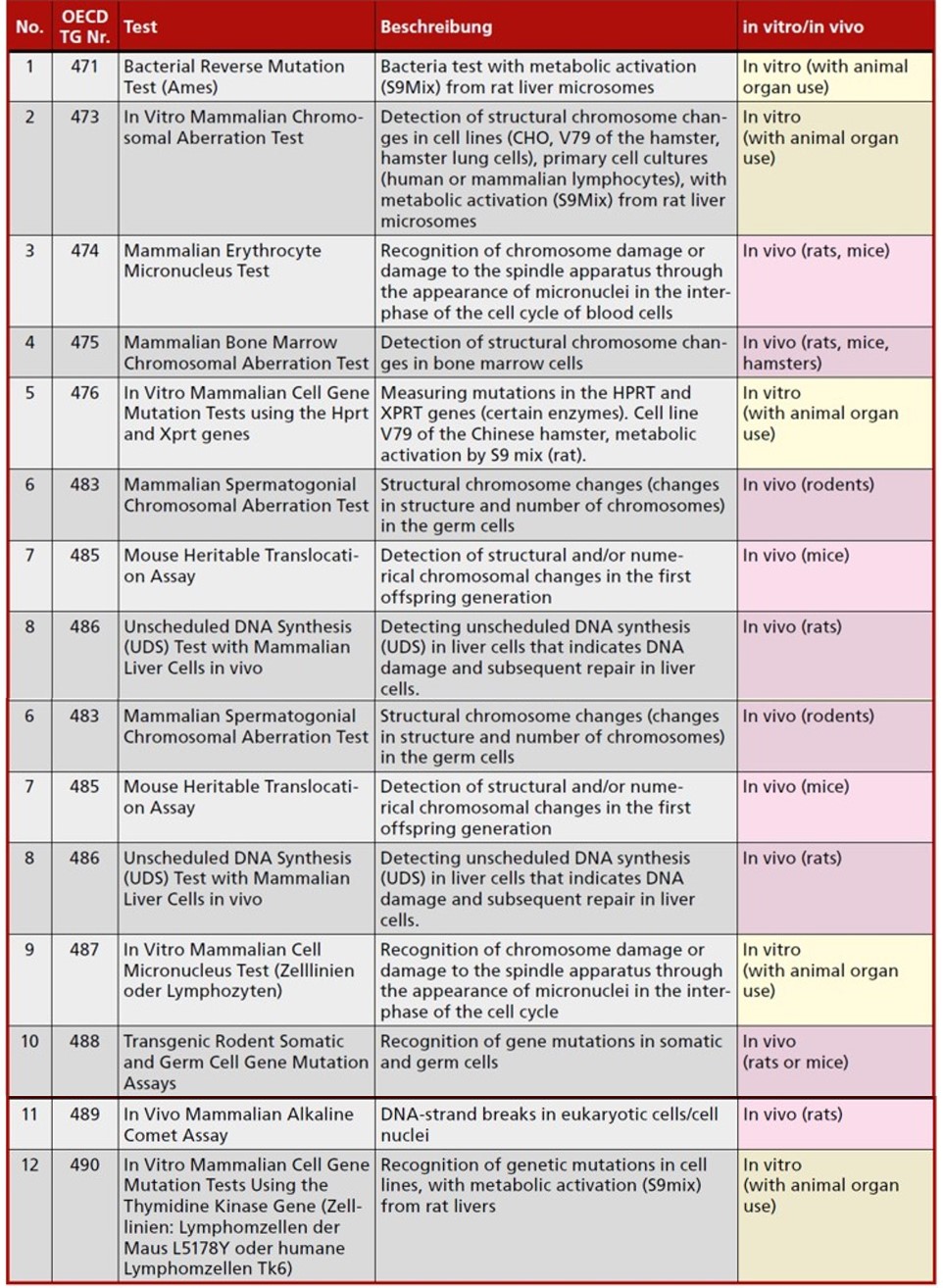
Gene mutation tests are used to determine whether a change takes place in a single gene, i.e. via a base substitution, deletion or insertion of a single base. Genome mutation tests examine changes in the entirety of all genes, i.e. via the change in the overall number of genes in the chromosome set.
Free from Animal Testing does not mean Free from Animal Suffering
Twelve different tests can be used for the study of DNA base changes or structural/numerical chromosome changes. None of these can be done without animals, even when five tests are carried out in vitro. The reason is that the metabolism in the cell cultures is only stimulated with the help of enzymes from rat livers (the so-called S9 mix). As a rule, rats are treated and poisoned with the substance Arochlor 1254, which was previously used as a flame retardant. After that, the animals are killed and their livers removed for isolation of an enzyme. Hence, these in vitro tests offer no alternative to animal suffering.
If the amount of a chemical produced in Europe per year is 1,000 tonnes or more, a test for carcinogenicity can be proposed by the registrant himself or requested by the European Chemicals Agency (ECHA) by following the REACH regulation, Annex X, in the course of the registration process. The latter is the case if the substance produced is widely distributed, there are indications of frequent or long-term human exposure or the substance is already classified as a Category 2 germ cell mutagen. Another reason is when animal studies with repeated administration (repeated dose) have shown that the substance can cause either an enlargement of an organ or tissue due to abnormal proliferation of cells14 or a possible or confirmed precursor of cancer (preneoplasia). If the substance has already been classified as germ cell mutagen of categories 1A or 1B, a carcinogenicity test does not need to be carried out.
During drug development, a study in rodents has to be carried out if there is evidence from laboratory studies, previous animal toxicity studies and human data indicating that the substance may have carcinogenic potential. The tests were introduced against the background that the drug in question would be taken regularly by the patient for at least six months.15
Legal Basis
The regulatory background regarding chemicals for preclinical testing on animals is provided by the REACH Regulation 1272/2008 on classification, labelling and packaging of substances and mixtures.
The foundations for the testing procedures are the OECD Testing Guidelines 451 (Carcinogenicity Studies) und 453 (Combined Chronic Toxicity-Carcinogenicity Studies).17
In drug development as well, animal experimentation is required i.e. in the Guidelines of the International Council for Harmonisation of Technical Requirements for Pharmaceuticals for Human Use (ICH) S1A, S1B, S1C(R2) as well as S2(R1).15, 18
Animal Experiments for Carcinogenicity Testing
Carcinogenicity studies take place after all other legally required animal experiments have been performed. If the test substance is a drug, the test process is already at the end of clinical phase 2.19
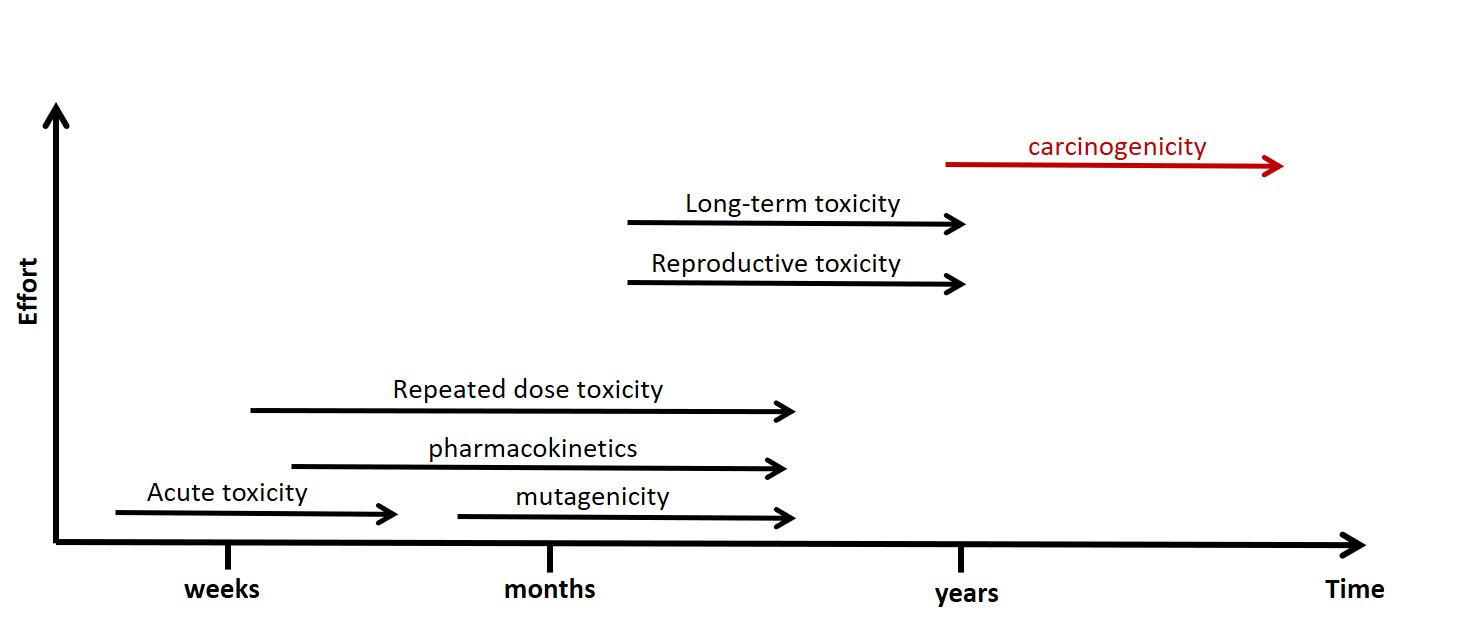
Fig. 1: Scheme of the stepwise strategy of toxicity tests.
Based on Aktories et al. (2009).13
The animal experiments are used to detect non-genotoxic carcinogens (for details, please refer to the box on genotoxicity, mutagenicity, carcinogenicity).10 The preferred species is the rat, but a different rodent species such as the mouse may be used as well. The reason for using these two species is their short life span and their susceptibility to tumors.16
Once they get to be two years of age, they are already relatively old, that is, the probability increases that the animals develop cancer. Therefore, carcinogenicity studies are run for two years. As with other mammals and humans, the immune system undergoes an aging process. An additional reason is that these animals, as the main species used in testing, are also used in other toxicological and pharmacological studies and therefore a lot of information about their physiology and pathology is available.16

Albino rat in the laboratory
Photo: Fotografixx, iStockphoto

Mice in Makrolon cages offering little stimulation
Photo: UnoL, iStockphoto
At least 500 Animals and more per Test
In carcinogenicity studies, both sexes of adult animals of a common laboratory strain are used. There are at least three dose groups and a control group. The doses are based on the results of the previous long-term or dose-finding studies. In each dose group, 50 animals are used, resulting in a total of at least 400 to 480 animals. However, to increase the statistical power, more animals can be used, especially in the low dose group, and also if the group sizes are no longer comparable due to deaths or removal for a necropsy. There may also be additional so-called sentinels (as a rule, 5 animals per gender). Sentinels are animals used to detect possible latent pathogens into the actual experimental animals.20 The aim is to rule out the possibility that a disease symptom can be traced back to a cause other than the test substance.
Daily poisoning for 24 Months
The rats and/or mice have to swallow the test substance regularly over a time period of two years. Alternatively, they receive an application to the skin or must inhale it, depending on how a person might be exposed to the chemical product later. The most common test route is, however, orally (by mouth). The administration takes place seven days a week, via the feed, drinking water or gavage (forced administration).
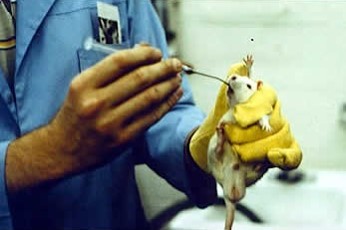
The substance is force-fed to a rat via gavage.
Photo: Peta2
If no data from previous long-term studies are available, 10 animals from each sex and dose group are eventually killed after one year and examined for neoplastic changes and mechanistic information. In this case, the original dose groups must be correspondingly larger. The majority, however, are sacrificed after 24 months, a necropsy performed, and the animals are checked to see if the animals have developed benign or malignant tumors.16
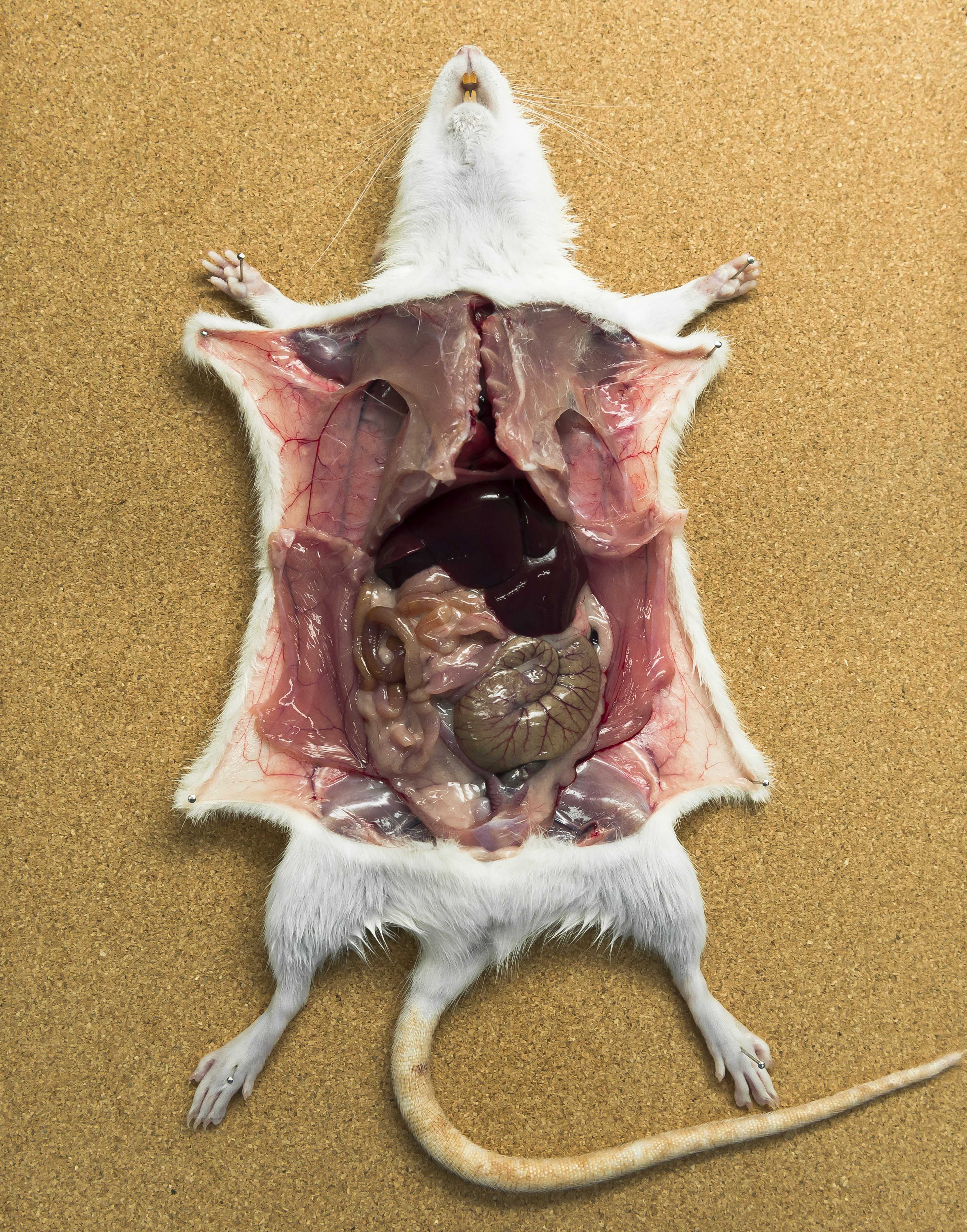
Rat prepared for necropsy
Photo: unoL, iStockphoto
The goal of the examinations is to check whether a given substance induces a higher incidence of neoplasias, a higher percentage of malignant tumors or a decrease in latency of appearance of neoplasias as compared to the control group. Besides, it is examined in which organs tumor development occurs and when. Also, it has to be clarified at which dose tumors develop and also the maximum dose that does not affect tumor generation (the so-called no-observed-adverse-effect level, NOAEL).
Test Frequency in Germany and Europe
The carcinogenicity tests have decreased in Germany and Europe in recent years, but have not been terminated.
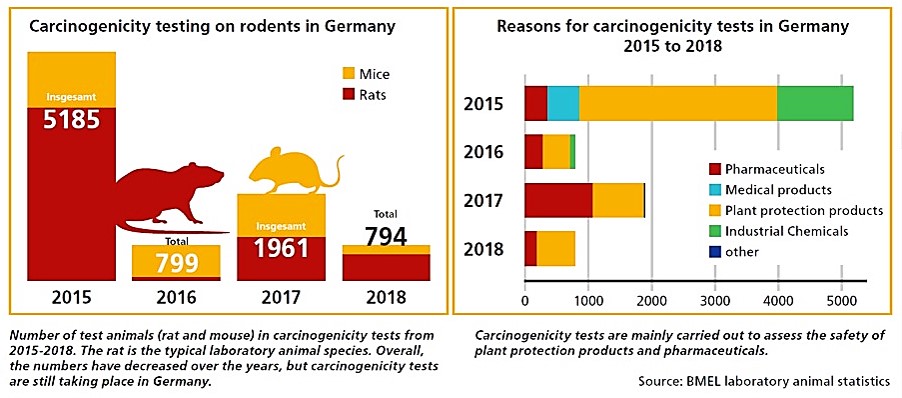
While in 2015 over 5,000 test animals suffered from carcinogenicity studies in Germany, their number decreased to less than 1,000 in 2018. Most recently, the tests were carried out exclusively for the manufacture of pharmaceuticals and pesticides. These are the products in which the end-user consumes the substance regularly and over the long term.
Across the EU, the number of laboratory animals used halved in 2017 compared to 2015 to 12,493. The European countries which still perform carcinogenicity studies are Germany, France, the Netherlands and the United Kingdom.
Criticism of the Animal Experiments
There are numerous criticisms of animal experiments, starting with the reproducibility of the results, continuing with the relevance of the animal studies, and extending to ethical considerations whether such stressful and long-lasting treatments are justifiable, especially in view of the unreliable results and redundancy.
Harm and Distress
According to the European Animal Experimentation Directive, Annex VIII11, the degree of distress in carcinogenicity studies can range from moderate to severe, especially in the case of induction of tumors or spontaneous tumors which can be expected to progressive and fatal including long-term moderate pain, distress or suffering. These include for example tumors causing wasting (cachexia), invasive bone tumors, metastatic tumors and tumors that are left to develop up to ulceration.
Tumor research is therefore often extremely stressful for animals. For this reason, during project planning, considerations and criteria on when to terminate an experiment are an absolute necessity (i.e. a certain tumor size, that is no longer tolerable for the animal). As a case study demonstrated21 in a first experiment, it took 75 days until the primary tumor had reached this size. In this time it had metastasized, and these metastases were explored. When the experiment was repeated, the tumor suddenly grew much faster and had reached its critical size after 45 days – not enough time to form metastases and adequately replicate the first study. Hence, we deal with biological variation, which cannot be influenced even by the most careful scientists.
Reproducibility
All scientific and medical progress is based on the reliability of published data. The pharmaceutical industry uses the findings to identify and further develop candidates for potential drugs. If, as in the following case, only 21 percent of the published literature can be fully replicated, this usually ends with the termination of the project, since further investments cannot be justified.22 This hinders drug development and leads to unnecessary animal use. Reproducibility is particularly poor in cancer research, in which highly stressful animal experiments are carried out.
The reproducibility crisis in cancer research – reasons and consequences
In 2011, Bayer Health Care reported that surprisingly often key results from published scientific articles, 70 percent from cancer research, could not be reproduced in-house. This impression was confirmed a year later by a systematic study of Amgen, which published that out of 53 studies barely 7 percent could be reproduced – in 47 cases this was not achieved. What does this mean for science, medicine, and, last but not least, laboratory animals?
The RP: CB project
The Reproducibility Project: Cancer Biology was launched in 2013 in response to these frightening discoveries to recreate and reproduce a total of 50 cancer studies. It is important to research the causes of the lack of reproducibility and, if possible, eliminate them. The authors of the original publications were asked to provide the original reagents and to disclose details of their methods. The results of the first 5 studies were published in 201724 and showed a mixed picture. Out of five studies, only two were able to reproduce the results of the preliminary studies. One was not reproducible, and two retries were rated as „not interpretable”.25 Other researchers26 were unable to reproduce four out of five studies, which is very close to the results of the Amgen study.27
The Reasons for the Lack of Reproducibility
These reasons can be divided into general ones (which apply to all research) and those which are specific to tumor research. Scientists from the University of Texas carried out an extensive survey.28 According to them, almost 55 percent of all researchers stated that they had not been able to reproduce the results of a scientific paper. The majority (almost 80 percent) then sought help from the original authors. Of these, almost 40 percent replied cooperatively, but the majority of those asked responded uncooperatively or not at all. This is scandalous since the scientist is of course responsible for his or her work and results and has to ensure that subsequent studies can build on them.
Internal dependencies are another problem: in a certain research group, dependent employees may care not to question the results of their superiors, even if their data do not support their hypothesis. The considerable pressure to publish do the rest so that data are published even if the authors themselves are not convinced of the validity of their data. In this way, peer pressure creates genuine „scientific myths“.
You have to make allowances for the fact that in research no paper dealing with complex issues and presenting several results is 100 percent replicable. For this, biology (of the cells or the test animals) is too complex and susceptible to failure. A failure rate such as this is, however, completely unacceptable. As stated above, especially in cancer research the reasons maybe not only lack of implementation and the pressure to publish, but biological reasons that are possibly not fully controllable. If this is the case, cancer research requires completely new methodologies.
Relevance
Evolution takes place also in the laboratory.(26) Animals, cells, and tumor cells change on an ongoing basis regards their genetic makeup. Since the mutations can mutually influence and build on one another, a tumor in one animal or at a certain time point may develop completely differently than in another animal or at a different time point. Accordingly, a poor reproducibility in cancer research would in some way be „intrinsic“ and could not be influenced. In animal experiments, the animals are injected with cancer cells that are (originally) all genetically identical. Depending on how long the tumor grows, the more it will differ in its genetic make-up and properties from the tumors in the other animals.
This could be a possible explanation for the fact that in the more recent studies of the RP: CB mentioned above, the three cell culture studies, but not the animal experiment, were reproducible; the cell culture experiments lasted from minutes to hours; the animal experiment two months. The relevance of such results for the human situation can at least be questioned.
Alternatives to Animal Testing for Carcinogenicity
Is there any other way to determine carcinogenicity without testing on animals?
For a long time, in vitro testing of known carcinogens failed because these substances go through a process of metabolic activation in the organism, which the early in vitro tests could not reproduce. An early breakthrough already in the late 1960s was the Ames test, providing for the first time a reliable correlation between mutagenicity in vitro and carcinogenicity in vivo.28 Nevertheless, enzymes from the rat liver are added to the cultures to boost metabolism.
From 2006 to 2012 the EU financed the CarcinoGENOMICS project in the 6th framework program with more than 10 million Euro. The aim was to be able to evaluate the carcinogenic potential of chemicals with a series of mechanism-based in-vitro tests as an alternative to tests for genotoxicity and carcinogenicity in rodents. Using in vitro models, primarily the reactions of the organs liver, lung, and kidney should be simulated. The so-called „omics“ technologies played a role. In toxicology, such ‚omics methodologies’ are used to assess substances, whether they induce changes in the entire genome, ultimately leading to the development of adverse effects.29 Omics technologies include genomics, proteomics, and metabolomics. While genomics look at the entirety of the genes of cells or living organisms, proteomics examines the totality of proteins and transcriptomics the active genes.30 When testing for substance-induced effects, the omics data can be used for substance class comparisons, predictions or discoveries.29 Phenotypic markers should be found, changes in gene expression and metabolic profiles identified, as well as ways to predict mechanisms of chemical carcinogenesis. The transcriptomic and metabolomic data obtained should be integrated into an in silico model of chemical carcinogenesis.31
In 2016, scientists of the Veterinary University of Hannover have already examined three highly evaluated in vitro tests (the BALB/c3T3–cell transformation assay, the Bhas42 cell transformation assay, and the embryo assay of the Syrian hamster) for their suitability as a substitute for carcinogenicity studies in rodents. According to the researchers, they can identify non-genotoxic carcinogens and are a useful addition to the in vitro genotoxicity test batteries (see below). At least they can markedly reduce animal testing because they can pre-select chemicals that have to be subjected to anyone in vivo carcinogenicity tests.32 The European validating authority EURL-ECVAM has validated two in vitro methods using Syrian hamster embryo (SHE)-cells with a mouse fibroblast cell line called BALB/c3T3. The tests can be found in the OECD Test Guidelines on the page Series on Testing and Assessment under the numbers 214 (from 2015) and 231 (from 2016).33 EURL-EVCAM recommends that the cell transformation assays, although they provide relevant information about the conversion potential of chemicals, should not be used as independent methods, but always in combination with other supplementary information sources as part of a weight of evidence approach or an integrated testing strategy.34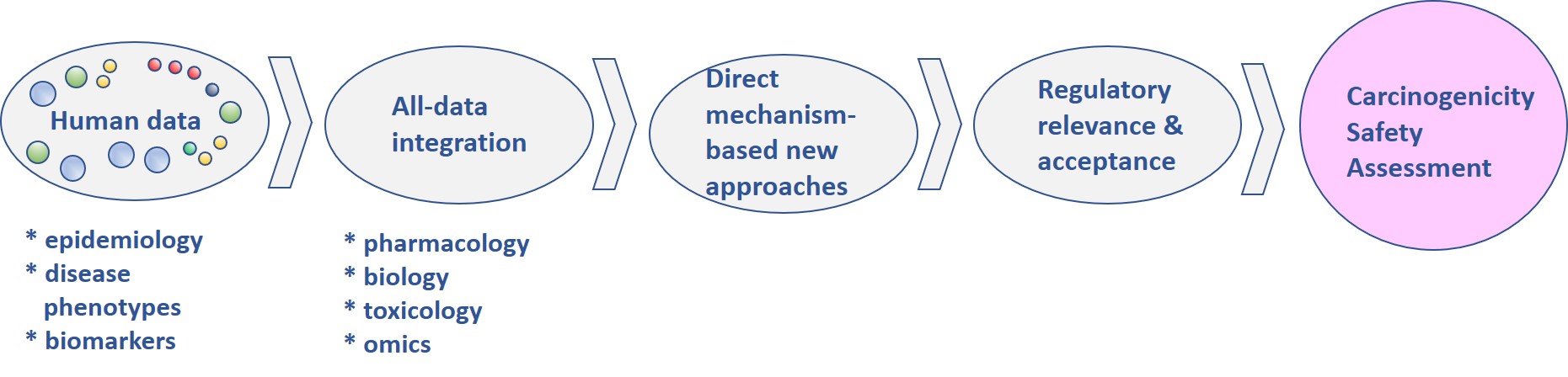
The integration of data, new technology applications and approaches in a tiered testing system should enable a better safety assessment of drugs and chemicals.
Graphik: Corvi et al. 2017. Toxicology In Vitro. (CC BY-SA 4.0)
There are also developments such as an in vitro method, with which carcinogens can be identified in human cell cultures. It is a culture with lymphoblastoid cells. Lymphoblastoid cell lines are genetically stable and serve as replacements for isolated or cryopreserved peripheral lymphocytes from the blood.35 In a five-year research project, scientists from Swansea University in Wales under Prof. Gareth Jenkins and Prof. Shareen Doakin tested such lymphoblastoid cells (TK636 and MCL-537) with eight known carcinogens and thereby achieved reliable results. Analyses comprised of chromosome damage, cell signaling, cell morphology, cell cycle dynamics, and bioenergetic disorders. Changes in cell morphology and gene expression have proven to be particularly suitable for the identification of environmental carcinogens.38 The approach can both be used for the detection of genotoxic and non-genotoxic carcinogens. However, questions still arise about whether they truly represent complex human organs and systems. Therefore the scientists aim to adapt the test with the help of 3D models of the human liver, skin, and lungs, to improve the closeness to the human physiology.39
According to the authors, the test could provide enough information to replace the two-year rodent carcinogenicity test for non-drugs and thus at least reduce the use of animals in this area.
No Two-year Carcinogenicity Study – Pharmacology, Genotoxicity, and Chronic Toxicity data are sufficient
Besides ethical and consistent political concerns about animal experiments, there are also practical needs for an approach other than the animal carcinogenicity test.40
As a result, in a workshop report 2017, ECHA and various stakeholders showed themselves convinced that in vitro genotoxicity tests together with the three- or six-month subchronic toxicity test in rats deliver sufficient data to assess the carcinogenicity risk of chemicals. Thus, the two-year study in rats can become obsolete.41
America's leading pharmaceutical research company (PhRMA), the American Food and Drug Administration (FDA), the Japan Pharmaceutical Manufacturers Association (JPMA) as well as the European Union have created a large number of data sets and analyzed retrospectively. They concluded that based on information on pharmacology, genotoxicity, and chronic toxicity (which are new drugs are usually available at the end of phase 2) the result of a 2-year study on carcinogenicity in rats can be predicted with reasonable certainty. Negative histopathology from a chronic rat study together with a negative result of genotoxicity and a negative result of a hormonal mechanism could be 82 percent accurate. However, this would only apply to about 30-40 percent of the compounds.19 An assessment of carcinogenicity without conducting a 2-year carcinogenicity study in rats can therefore only be made for certain pharmaceuticals. Additionally, this does not apply to biotechnologically produced medicinal products that follow the ICH S6(R1) guide.16
The European Medicines Agency (EMA) also has access to this information, a waiver could be possible: A so-called Regulatory Note on Amendments to the Core Guideline ICH S1 on the Testing of Carcinogenicity of Medicinal Products in Rodents“ (EMA/CHMP/ICH/536328/2013 Rev. 1) cautiously deals with a possible waiver of this animal studies. An ICH S1 Expert Working Group (S1 EEC) has evaluated data sets and concluded that knowledge of pharmacological information, together with toxicological and other data, may in certain cases provide sufficient information to predict the outcome of two-year rat carcinogenicity studies and their potential value in predicting the risk of human carcinogenicity of a given drug.42 The regulatory note was adopted on 25 February 2016.
The OECD also announces an integrated approach for the testing and evaluation of non-genotoxic carcinogens (IATA).43 Although there is a series of in vitro genotoxicity tests, the lack of human relevance being demonstrated by an in vivo test on rodents leaves an information gap, which the OECD has filled with an integrated testing strategy. Jacobs et al (2020) have developed here a draft version.44 Helpful here, among other things, are the adverse Outcome Pathways (AOPs), existing knowledge of toxicity mechanisms on different levels of biological organization, which ultimately lead to the health effect (tumor development). The integrated testing strategy (IATA) is to be applied to human cells and tissues that best replicate the human in vivo situation. Due to the variety of cell mechanisms, a whole series of such tests is necessary. At present, however, the cell systems are not yet sufficiently developed. From this basically, the first IATA draft considers also still different mammalian cell systems and tests over three or seven days or 28 and 90 days on animals. The testing strategy shall but continue to evolve and adapt to the state of scientific knowledge and developments can be adapted bit by bit. The rodent carcinogenicity test should not find consideration.42
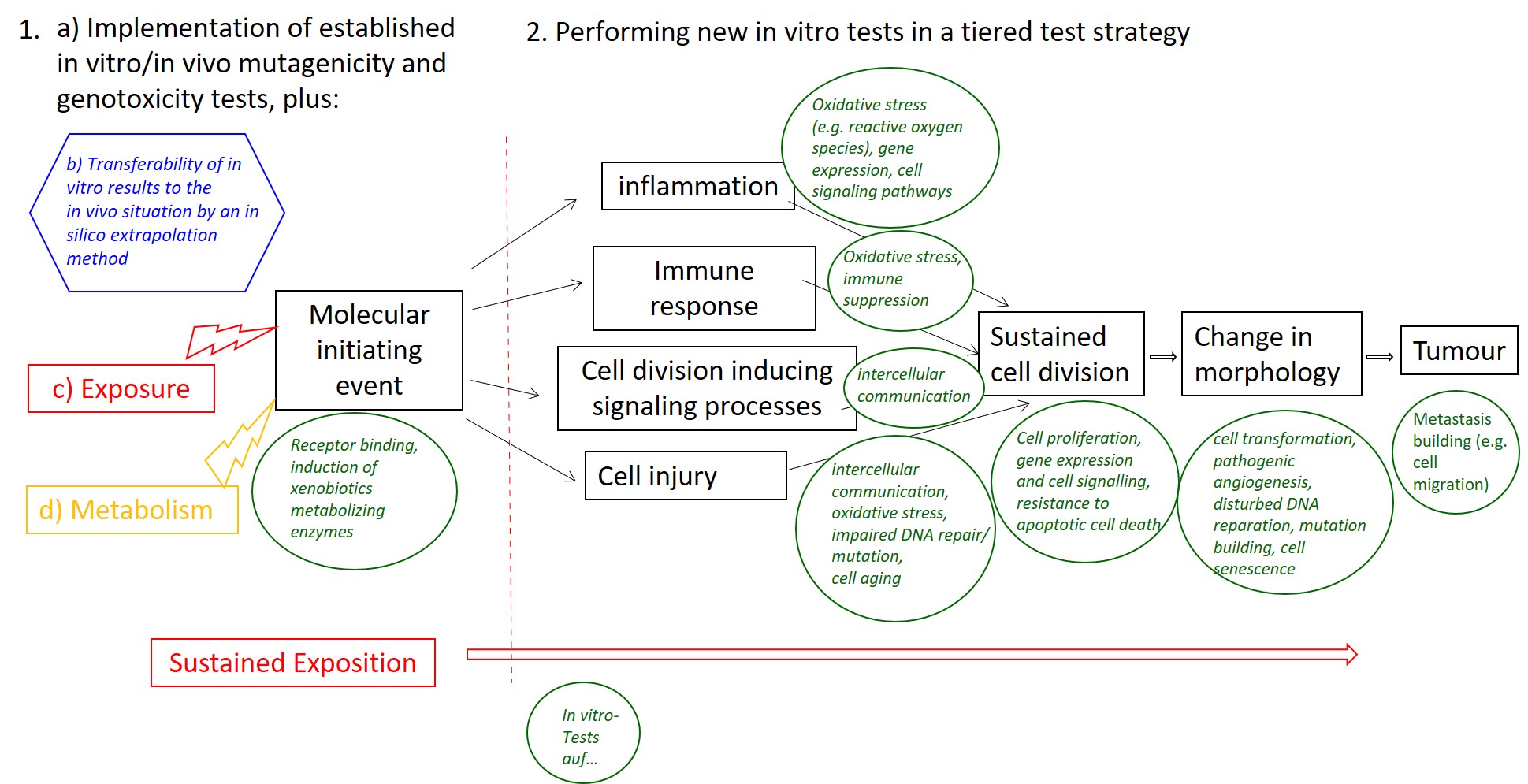
Integrated testing strategy design for testing non-genotoxic carcinogens, here simplified. First of all, established in vitro and in vivo genotoxicity and mutagenicity tests are carried out and used with additional information on metabolism (yellow) and exposure (red) and an extrapolation method on the computer (blue) for the first risk assessment. In cases of long-term exposure (red below) to the environmental substance to be examined, a large number of individual tests are used (in green circles), some of which still have to be developed. The individual steps to tumor formation correspond to the cascade of events as described in the Adverse Outcome Pathway concept. The in vitro tests are combined with further tests for epigenetic changes.
Chart according to Jacobs et al. Archives of Toxicology (2020) 94: 2899-2923, slightly simplified.
Outlook
There is an engagement i.e. from the European Partnership for Alternative Approaches to Animal Testing (EPAA): 35 companies from the sectors animal health, chemicals, cosmetics, crop protection, fragrances, pharmaceuticals, soaps, and cleaning agents as well as five directorates of the European Commission, among others the Joint Research Center with the European validation authority ECVAM have joined forces.41 The EPAA's steering group is made up of members from industry and commission representatives and is advised by a mirror group consisting of experts from science, animal welfare, representatives from the fields of animal experimentation, and other organizations. With its action programs, EPAA focuses on the implementation of new methods to replace animal experiments and aims to promote the regulatory acceptance of the methods, including those for carcinogenicity testing.41 The ultimate aim of the EPAA is to have access to testing methods for the decision-making in the regulatory sector that are scientifically robust, faster, and less expensive than tests on animals.
Based on research results and an EPAA workshop back in 2013, scientific evidence was to be collected in an expanded database. The aim was to convince the regulatory authorities to accept the waiver of the two-year carcinogenicity study in rats. For this purpose, 364 chemical compounds were documented in a freely accessible database (TOXRef) at the University of Wageningen.41 Interestingly, the study was part of a package that intended to comprise equally pharmaceuticals, their additives, and chemicals (mainly agrochemicals).41 A peer-reviewed publication containing the conclusions of this database is expected to be delivered shortly. Based on this publication, a team from EPAA and the European Federation of Pharmaceutical Industries and Associations (EFPIA) want to develop a concept paper that will be presented at the next ICH conference and aims to agree on concrete steps for discussions with the regulatory authorities.
Most conventional test results are descriptive and do not provide information about the sequence of events in cells and tissues that can lead to cancer development. That is why scientists, industry, and regulatory authorities are now working on a so-called mechanistic approach, which was presented by the American regulatory authorities in the publication „Toxicity in the 21st Century – a Vision and a Strategy” in the Year 2009. The accuracy and the possibility of high throughput approaches save costs and time. Information systems have evolved and are now able to process billions of data at once, which could be exchanged internationally and provide important information.40
The tumor formation can be also be predicted better using mechanistic information. Therefore, experts proposed an alternative, mechanistic approach to cancer risk assessment of agrochemicals.45 The new procedure envisages combining results from test methods for the detection of modes of action of non-genotoxic carcinogenicity with information from subchronic toxicity studies. Gradually, in silico, in vitro and short-term in vivo models could be used to identify the various action modes involved in tumor development. The participants consider the approach realistic and therefore a continuous dialogue between all stakeholders shall build confidence in the proposed approach and its scientific accuracy. In the coming years, the regulatory implementation shall be promoted.
References
(1) https://echa.europa.eu/de/substance-information/-/substanceinfo/100.005.779
(2) Europäische Union (2017). Durchführungsverordnung (EU) 2017/244 der Kommission vom 10. Februar 2017 zur Nichterneuerung der Genehmigung für den Wirkstoff Linuron gemäß der Verordnung (EG) Nr. 1107/2009 des Europäischen Parlaments und des Rates über das Inverkehrbringen von Pflanzenschutzmitteln und zur Änderung des Anhangs der Durchführungsverordnung (EU) Nr. 540/2011 der Kommission.
https://eur-lex.europa.eu/legal-content/DE/TXT/PDF/?uri=CELEX%3A32017R0244
(3) https://www.euro.who.int/__data/assets/pdf_file/0020/185312/Leading-causes-of-death-in-Europe-Fact-Sheet-Ger.pdf
(4) https://www.destatis.de/DE/Themen/Gesellschaft-Umwelt/Gesundheit/Todesursachen/todesfaelle.html
(5) https://www.bundesgesundheitsministerium.de/themen/praevention/gesundheitsgefahren/krebs.html
(6) Marquardt, H., Schäfer, S. & Barth, H. (2013). Toxikologie. 3. Auflage, Stuttgart.
(7) Bundesinstitut für Risikobewertung (2020). Risikobewertung von Pflanzenschutzmitteln.
https://www.bfr.bund.de/de/risikobewertung_von_pflanzenschutzmitteln-70187.html
(8) https://www.nanopartikel.info/
(9) DocCheck Flexikon (2020). Kanzerogen. https://flexikon.doccheck.com/de/Kanzerogen
(10) Jacobs, M. N., Colacci, A., Louekari, K., Luijten, M., Hakkert, B. C., Paparella, M. & Vasseur, P. (2016). International Regulatory Needs for Development of an IATA for Non-Genotoxic Carcinogenic Chemical Substances. ALTEX 33(4): 359-392.
(11) Richtlinie 2010/63/EU des Europäischen Parlaments und des Rates vom 22. September 2010 zum Schutz der für wissenschaftliche Zwecke verwendeten Tiere. https://www.bfr.bund.de/cm/343/5_Beratung_Anlage%203_2010-63-EU.pdf
(12) https://www.bundesgesundheitsministerium.de/themen/praevention/gesundheitsgefahren/krebs.html
(13) Aktories, K., Förstermann, U., Hofmann, F. & Starke, K. (2009). Allgemeine und spezielle Pharmakologie und Toxikologie. Urban & Fischer Verlag, München.
(14) DocCheck Flexikon (2020). Hyperplasie. https://flexikon.doccheck.com/de/Hyperplasie
(15) European Medicines Agency (2020). ICH S1A The Need for Carcinogenicity Studies of Pharmaceuticals.
https://www.ema.europa.eu/en/ich-s1a-need-carcinogenicity-studies-pharmaceuticals
(16) OECD library (2018). OECD Guidelines for the Testing of Chemicals, Section 4, Health effects, Test No. 451: Carcinogenicity Studies.
https://www.oecd-ilibrary.org/
(17) https://www.oecd-ilibrary.org/
(18) Bundesinstitut für Arzneimittel und Medizinprodukte (2020). The International Council for Harmonisation of Technical Requirements for Pharmaceuticals for Human Use (ICH). https://www.bfarm.de/DE/BfArM/EU_Internationales/ICH/_node.html
(19) European Medicines Agency (2016). ICH guideline S1, Regulatory notice on changes to core guideline on rodent carcinogenicity testing of pharmaceuticals. EMA/CHMP/ICH/536328/2013 Rev. 1, Committee for Human Medicinal Products, 29 February 2016. https://www.ema.europa.eu/en/documents/
(20) Gesellschaft für Versuchstierkunde GV-Solas (2009). Hygiene-Überwachung von Maus- und Rattenbeständen bei verschiedenen Haltungsformen. http://www.gv-solas.de/fileadmin/user_upload/pdf_publikation/Hygiene/hyg-ueberw_maus-ratte.pdf
(21) Friedl, P. (2019). Rethinking research into metastasis. eLife 8:e53511. DOI: https://doi.org/10.7554/eLife.53511
(22) Prinz, F., Schlange, T. & Asadullah, K. (2011). Believe it or not: how much can we rely on published data on potential drug targets? Nat Rev Drug Discov 10, 712. https://doi.org/10.1038/nrd3439-c1
(23) Errington, T.M., Iorns, E., Gunn, W., Tan, F.E., Lomax, J. & Nosek, B.A. (2014). An open investigation of the reproducibility of cancer biology research. Elife 3:e04333. doi:10.7554/eLife.04333
(24) Nosek, B. A.& Errington, T. M. (2017). Reproducibility in Cancer Biology. Making sense of replications. eLife 2017, 6:e23383. DOI: 10.7554/eLife.23383
(25) Baker, M., Dolgin, E. (2017). Reproducibility project yields muddy results. Nature 541: 269–270. https://www.nature.com/
(26) Wen, H., Wang, H.-Y., He, X. & Wu, C.-I. (2018). On the low reproducibility of cancer studies. National Science Review 5/5: 619–624.
https://doi.org/10.1093/nsr/nwy021
(27) Begley, C., Ellis, L. (2012). Raise standards for preclinical cancer research. Nature 483, 531–533. https://doi.org/10.1038/483531a
(28) Mobley, A., Linder S. K., Braeuer, R., Ellis, L. M. & Zwelling, L. (2013). A Survey on Data Reproducibility in Cancer Research Provides Insights into Our Limited Ability to Translate Findings from the Laboratory to the Clinic. PLOS ONE 8/5, e63221. https://doi.org/10.1371/journal.pone.0063221
(29) Sauer, U. G., Deferme, L., Gribaldo, L., Hackermüller, J., Tralau, T., van Ravenzwaay, B., Yauk, C., Poole, A., Tong, W. & Gant, T. W. (2017). The challenge of the application of 'omics technologies in chemicals risk assessment: Background and outlook. Regulatory Toxicology and Pharmacology 91: S14-S26.
(30) https://ekvv.uni-bielefeld.de/blog/uniaktuell/entry/omics_technologien_teilen
(31) European Commission (Last update: 26 March 2013). Development of a high throughput genomics-based test for assessing genotoxic and carcinogenic properties of chemical compounds in vitro. https://cordis.europa.eu/project/id/37712
(32) Steinberg, P. (2016). In Vitro–In Vivo Carcinogenicity. Adv Biochem Eng Biotechnol, DOI: 10.1007/10_2015_5013
(33) http://www.oecd.org/chemicalsafety/testing/series-testing-assessment-publications-number.htm
(34) https://ec.europa.eu/jrc/en/eurl/ecvam/alternative-methods-toxicity-testing/validated-test-methods/carcinogenity/three-cta
(35) Hussain, T. & Mulherkar, R. (2012). Lymphoblastoid Cell lines: a Continuous in Vitro Source of Cells to Study Carcinogen Sensitivity and DNA Repair. Int J Mol Cell Med 1/2: 76-87. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3920499/
(36) https://www.sigmaaldrich.com/
(37) Crespi, C. L., Gonzales, F. J., Steimel, D. T. et al. (1991). A Metabolically Competent human Cell line Expressing Five cDNA Encoding Procarcinogen-Activating Enzymes: Application to Mutagenicity Testing. Chem. Res. Toxicol. 4: 566-572. https://pubs.acs.org/doi/abs/10.1021/tx00023a013
(38) Wilde, E.C., Chapman, K.E., Stannard, L.M. et al. (2018). A novel, integrated in vitro carcinogenicity test to identify genotoxic and non-genotoxic carcinogens using human lymphoblastoid cells. Arch Toxicol 92, 935–951. https://doi.org/10.1007/s00204-017-2102-y
(39) Jenkins, G. & Doak, S. (2018). Breakthrough could end animal testing in carcinogen research. https://theconversation.com/
(40) Paparella, M., Colacci, A. & Jacobs. M. N. (2017). Uncertainties of testing methods: What do we (want to) know about carcinogenicity? ALTEX 34(2): 235-252. doi: 10.14573/altex.1608281. Epub 2016 Oct 24. PMID: 27776202.
(41) European Chemicals Agency (ECHA) (2016). New Approach Methodologies in Regulatory Science. Proceedings of a scientific workshop Helsinki, 19–20 April 2016. https://echa.europa.eu/documents/10162/22816069/scientific_ws_proceedings_en.pdf
(42) https://www.ema.europa.eu/
(43) OECD (2020). Overview of Concepts and Available Guidance related to Integrated Approaches to Testing and Assessment (IATA), OECD Series on Testing and Assessment, No. 329, Environment, Health and Safety, Environment Directorate, OECD.
(44) Jacobs MN, Colacci A, Corvi R, Vaccari M, Aguila MC, Corvaro M, Delrue N, Desaulniers D, Ertych N, Jacobs A, Luijten M, Madia F, Nishikawa A, Ogawa K, Ohmori K, Paparella M, Sharma AK, Vasseur P. Chemical carcinogen safety testing: OECD expert group international consensus on the development of an integrated approach for the testing and assessment of chemical non-genotoxic carcinogens. Arch Toxicol. 2020 Aug;94(8):2899-2923. doi:10.1007/s00204-020-02784-5. Epub 2020 Jun 27. PMID: 32594184; PMCID: PMC7395040.
(45) Luijten, M., Corvi, R., Mehta, J., Corvaro, M., Delrue, N., Felter, S., Haas, B., Hewitt, N. J., Hilton, G., Holmes, T., Jacobs, M. N., Jacobs, A., Lamplmair, F., Lewis, D., Madia, F., Manou, I., Melching-Kollmuss, S., Schorsch, F., Schütte, K., Sewell, F., Strupp, C., van der Laan, J. W., Wolf, D. C., Wolterink, G., Woutersen, R., Zvonar, Z., Heusinkveld, H. & Braakhuis, H. (2020). A comprehensive view on mechanistic approaches for cancer risk assessment of non-genotoxic agrochemicals. Regul Toxicol Pharmacol. 118: 104789. doi: 10.1016/j.yrtph.2020.104789. Epub ahead of print. PMID: 33035627.




 Dr. rer. nat.
Dr. rer. nat. Menschen für Tierrechte - Tierversuchsgegner Rheinland-Pfalz e.V.
Menschen für Tierrechte - Tierversuchsgegner Rheinland-Pfalz e.V.